About Us
About UsWe didn’t set out to build another app or a SaaS tool. We aren’t an AI bot looking for a use case. We’re a small team rebuilding health insurance from the ground up.
For businesses
For employees
For Brokers
AT A GLANCE
What Is Arlo

How health insurance works
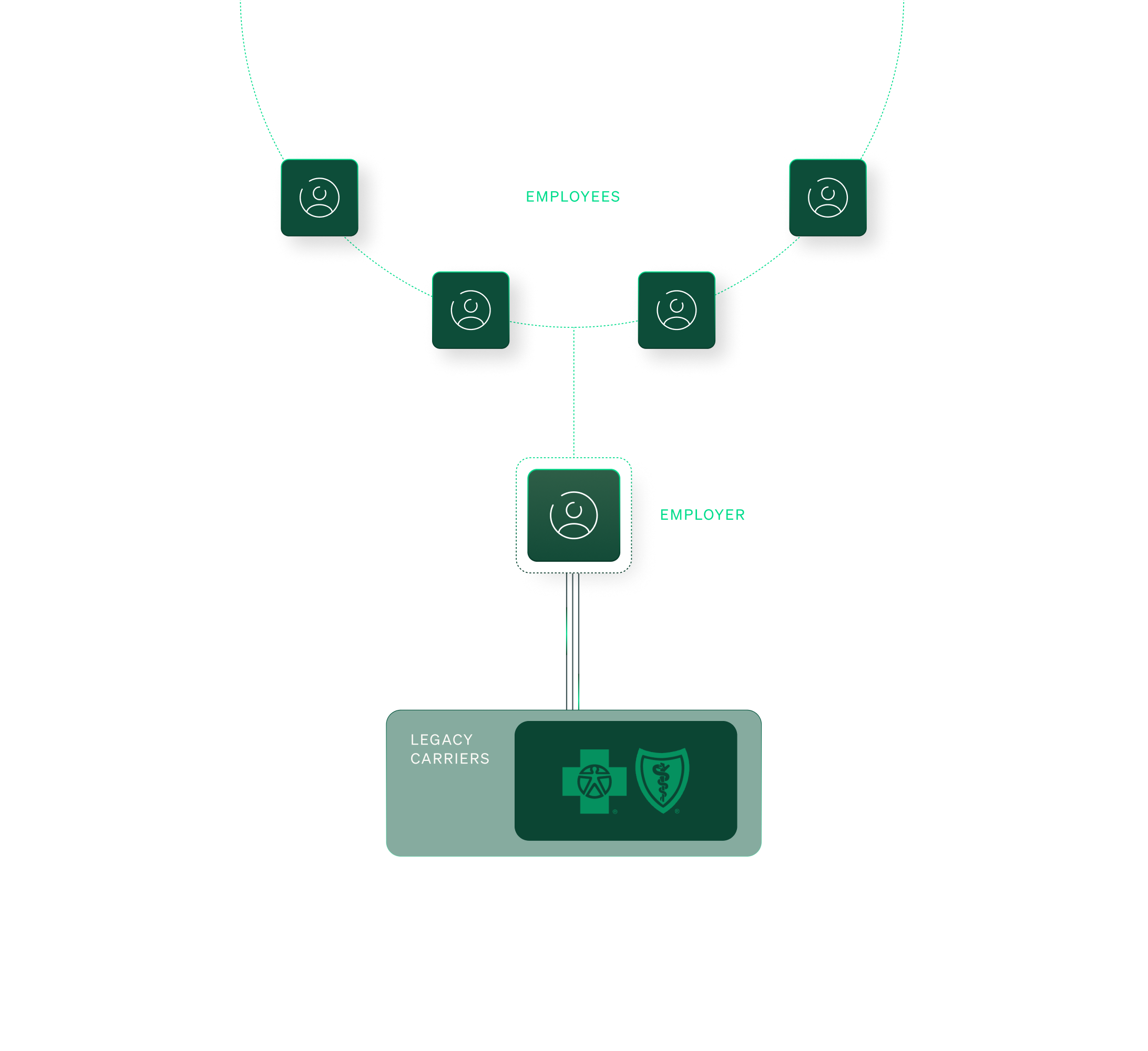
How health insurance works
Most people get health insurance through their employer. And most employers don't have much choice. They are stuck picking between a handful of large carriers: the Blues, United, Cigna, Aetna.
The problem
The problem
These carriers are really good at one thing: processing claims. But they've underinvested in everything else. The patient experience is poor. The infrastructure to actually help people get good care doesn't exist. So they compete on price, and the easiest way to keep prices down is to make care harder to access.
What we're building
What we're building
We started Arlo to rethink how health insurance should work. We built our own health plan, underwrite it ourselves, support our members directly, and build all the technology behind it. We're combining engineering, product, and data science to drive down costs in ways that don't involve making care harder to get.
Where we are
Where we are
In less than two years, we've scaled to cover tens of thousands of lives and hundreds of businesses. We've hit profitability with a small, focused team, and we're just getting started. Our goal is 1 million lives in the next 5 years—join us for the build.


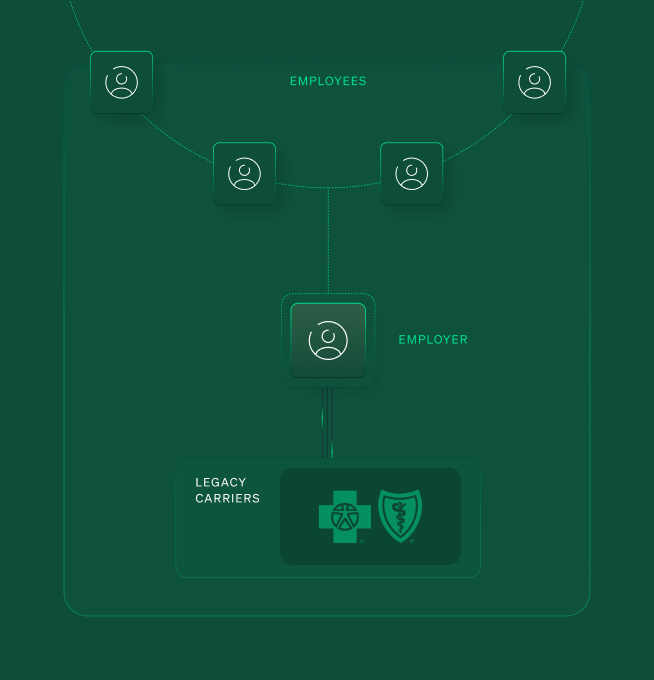
How health insurance works
Most people get health insurance through their employer. And most employers don't have much choice. They are stuck picking between a handful of large carriers: the Blues, United, Cigna, Aetna.

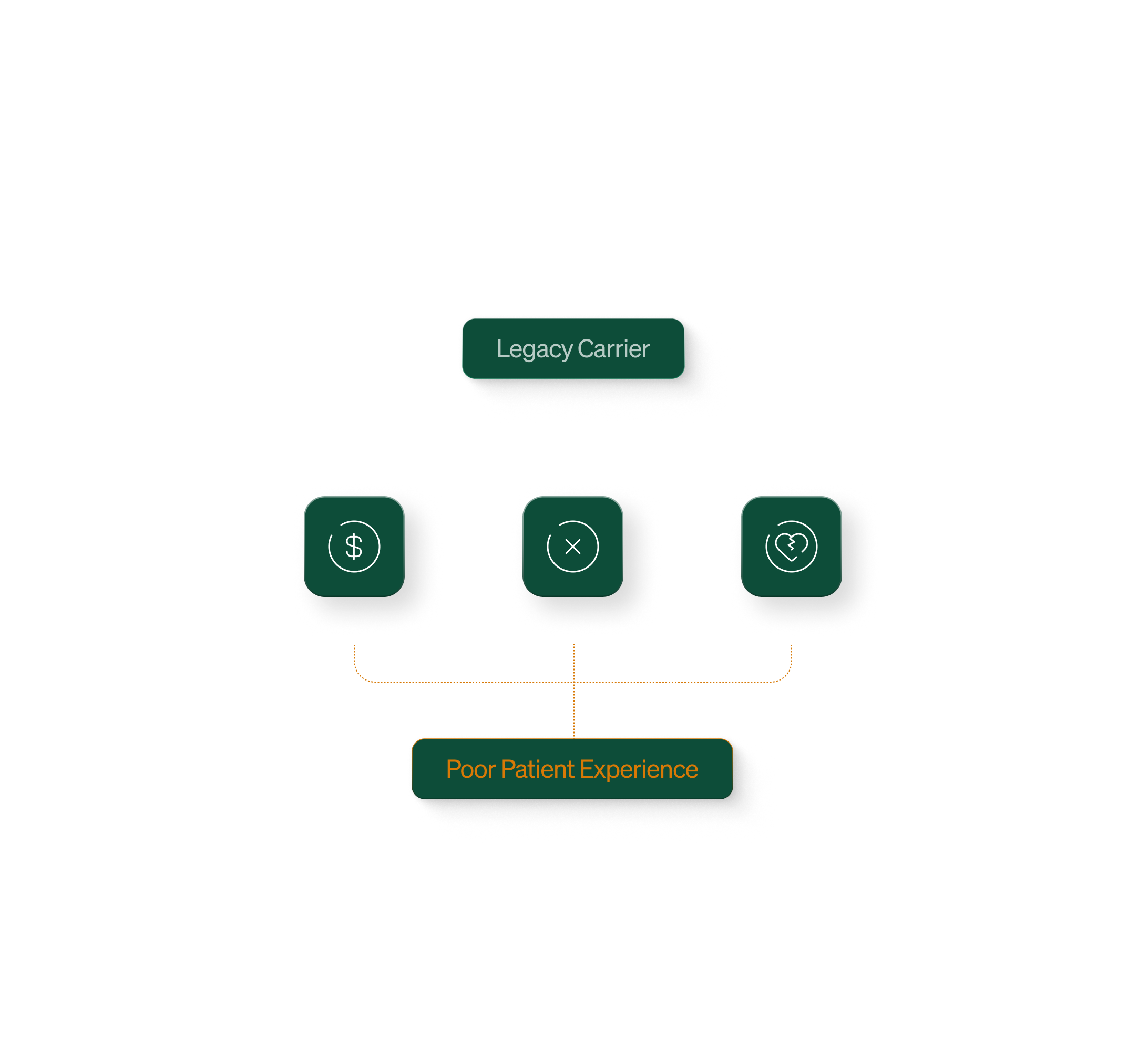
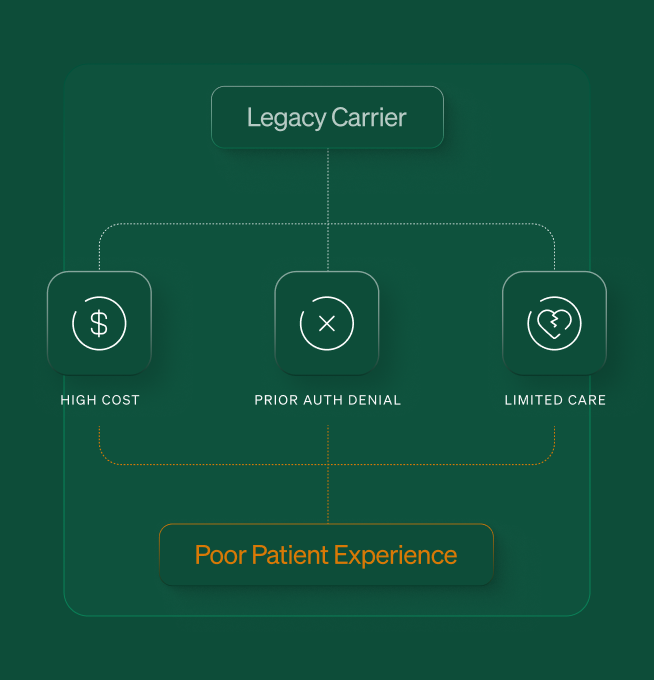
The problem
These carriers are really good at one thing: processing claims. But they've underinvested in everything else. The patient experience is poor. The infrastructure to actually help people get good care doesn't exist. So they compete on price, and the easiest way to keep prices down is to make care harder to access.


What we're building
We started Arlo to rethink how health insurance should work. We built our own health plan, underwrite it ourselves, support our members directly, and build all the technology behind it. We're combining engineering, product, and data science to drive down costs in ways that don't involve making care harder to get.


Where we are
In less than two years, we've scaled to cover tens of thousands of lives and hundreds of businesses. We've hit profitability with a small, focused team, and we're just getting started. Our goal is 1 million lives in the next 5 years—join us for the build.
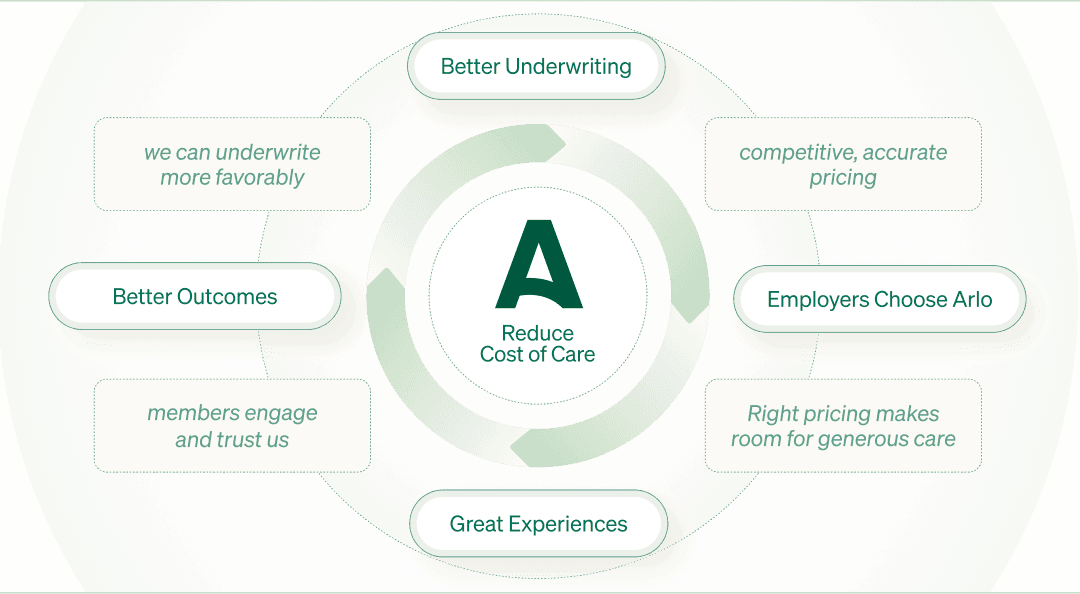
ARLO FLYWHEEL
What We're Building
Every team here feeds into the next. We've shipped a lot in a short time, and we're just getting started.

What We Shipped
We rebuilt our underwriting model and risk engine from scratch. What was a multi-week email process is now a single API call.
What’s Next
In 2026, we’re expanding and refining this foundation by improving risk signals, increasing model transparency, and making the system more adaptive over time.
Who Drives It
This is owned by our data science, data engineering, and actuarial teams who work hand-in-hand, bringing deep healthcare expertise and modern ML and engineering.

What We Shipped
A small sales team has brought on hundreds of brokerages and quoted tens of thousands of businesses—powered by a quoting portal that brokers actually prefer over incumbents.
What’s Next
We're 5xing our sales team and embedding our quoting software into payroll systems and other channels to accelerate distribution.
Who Drives It
This is owned by our sales and engineering teams - experienced leaders from top insurers and brokerages, alongside engineers building the portal and APIs.

What We Shipped
A mobile app that serves as a care guide for our members making it easier to access virtual care, order labs, and refill prescriptions. Our CX team backs it up with a 95%+ CSAT.
What’s Next
We're building an AI care guide that makes accessing healthcare incredibly easy and supports members outside the four walls of the clinic.
Who Drives It
This is owned by our engineering, product, design, and customer support teams who are all obssessed with creating pixel-perfect patient experiences.

What We Shipped
Experiences that increase price transparency, guide members to higher-value providers, and encourage preventive and mental health care, reducing claims costs and improving outcomes.
What’s Next
We're building out our clinical team, launching chronic condition management programs, and working with engineering to design proactive AI care guides that help members stay on top of their health.
Who Drives It
This is owned by our product and clinical teams.
MEET











































